What Is Immunotherapy?
Immunotherapy is a treatment approach that harnesses the body’s natural defense system— the immune system— to fight cancer and certain other diseases. Also referred to as “biological therapy,” it is designed to either stimulate or restore the immune system’s ability to detect and destroy abnormal cells, particularly cancer cells.
The immune system is a complex network consisting of white blood cells, lymph nodes, the spleen, and bone marrow. Under normal conditions, it can identify and eliminate harmful invaders, including cancerous cells. However, cancer cells can sometimes evade or suppress immune responses. Immunotherapy helps re-enable and enhance the immune system’s ability to recognize and attack these abnormal cells.
How Does Immunotherapy Work Against Cancer?
Cancer cells often develop sophisticated mechanisms to escape immune detection. For instance, they may:
- Release proteins that suppress immune cells,
- Alter the surrounding healthy tissues to interfere with immune signaling,
- Express surface proteins that mimic normal, healthy cells.
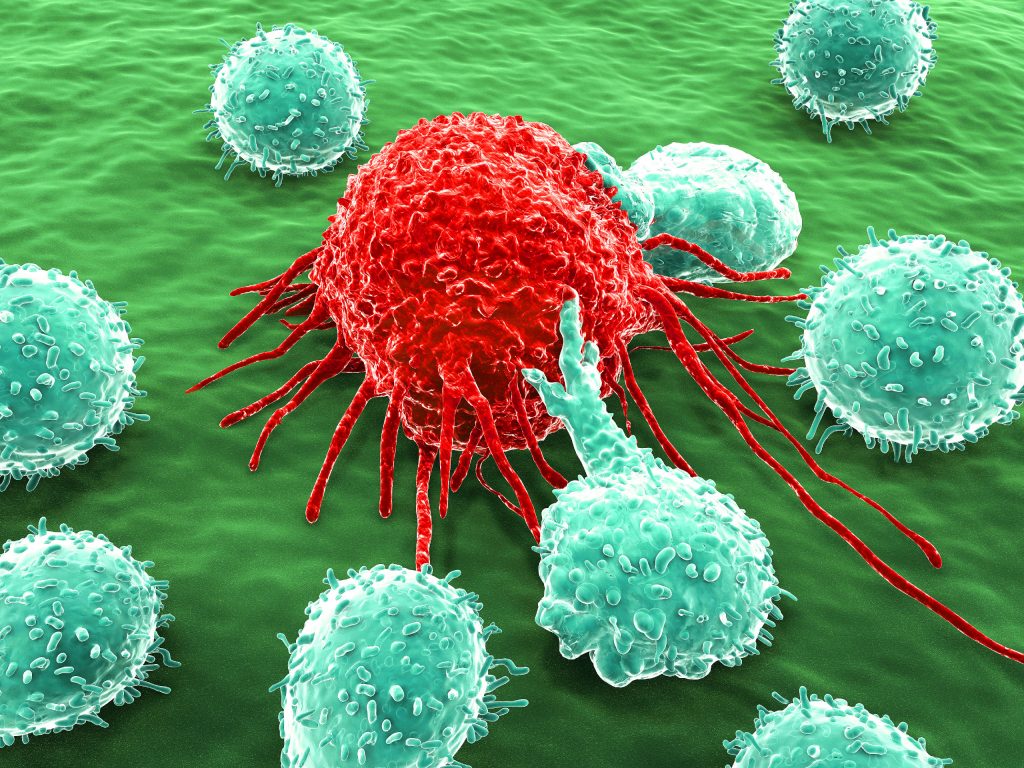
Immunotherapy intervenes by disrupting these escape mechanisms. This reactivates immune cells and enables them to effectively recognize, target, and destroy cancer cells.
Types of Immunotherapy
1. Immune Checkpoint Inhibitors
Immune checkpoints are natural regulators of the immune system, acting as brakes to prevent overactivity. Cancer cells exploit these checkpoints to shut down immune responses. Checkpoint inhibitors block these brakes, allowing immune cells—especially T cells—to remain active and attack tumors.
Common Uses: Lung cancer, melanoma, bladder cancer, kidney cancer, and head & neck cancers.
2. T-Cell Transfer Therapy (Adoptive Cell Therapy)
This involves collecting immune cells (usually T cells) from a patient’s tumor, modifying or enhancing them in the lab, and reinfusing them into the patient.
Subtypes include:
- TIL (Tumor-Infiltrating Lymphocytes) Therapy
- CAR-T Cell Therapy: T cells are genetically engineered to express specific receptors (CARs) that better recognize and attack cancer cells.
3. Monoclonal Antibodies (mAbs)
These are laboratory-produced antibodies that bind to specific targets (antigens) on cancer cell surfaces.
Functions include:
- Direct cancer cell destruction,
- Immune system recruitment,
- Blocking growth signals.
4. Cancer Vaccines
Therapeutic cancer vaccines are designed to stimulate the immune system to recognize and attack cancer-specific antigens.
Goal: Train the immune system to identify and destroy cancer cells.
5. Immune System Modulators (Cytokines)
These therapies enhance the general activity of the immune system.
Examples:
- Interferon-alpha (IFN-α): Inhibits cancer cell growth.
- Interleukin-2 (IL-2): Boosts T cell and NK cell production.
- BCG Therapy (for bladder cancer): Triggers a localized immune response.
Which Cancers Can Be Treated with Immunotherapy?
While immunotherapy is not yet applicable to all cancers, it has proven effective in several types:
- Non-small cell lung cancer
- Melanoma
- Bladder cancer
- Renal cell carcinoma
- Lymphomas (especially Hodgkin lymphoma)
- Head and neck cancers
- Selected cases of liver, gastric, colorectal, and breast cancers
Treatment suitability is assessed based on individual genetic and immunological profiles, often using biomarker tests.
Side Effects of Immunotherapy
Since immunotherapy can activate immune cells against healthy tissues, side effects may occur. Common reactions include:
- Fatigue
- Diarrhea
- Skin rashes or itching
- Flu-like symptoms
- Inflammation of organs (e.g., lungs, intestines, thyroid, liver)
Less common but serious side effects:
- Cytokine release syndrome
- Neurological complications
- Capillary leak syndrome
- Severe allergic reactions
Monitoring by experienced oncologists and immunologists is essential throughout the treatment process.
How Is Immunotherapy Administered?
Immunotherapy may be delivered through various routes, depending on the drug and cancer type:
- Intravenous (IV) infusion
- Oral tablets or capsules
- Topical application (creams)
- Intravesical (directly into the bladder)
The frequency and duration of treatment depend on the specific therapy, cancer stage, and patient response. Some regimens follow a cycle of administration and rest periods.
How Is Treatment Response Measured?
The success of immunotherapy is usually evaluated by:
- Physical examinations
- Imaging tests (CT, MRI, PET-CT)
- Blood tests
Because every patient’s immune system reacts differently, the time it takes to observe a response may vary. Some patients may experience early improvement, while others show delayed benefits.
Conclusion: A Promising Future in Cancer Care
Immunotherapy represents a transformative advance in cancer treatment. It offers a targeted, often less toxic alternative to traditional treatments and can create long-lasting immune memory that helps prevent recurrence.
Although not suitable for everyone, immunotherapy provides hope—especially for patients with resistant or advanced cancers. When carefully selected and properly managed, it can offer a powerful, personalized approach to cancer care.
✅ Frequently Asked Questions (FAQ) About Immunotherapy
❓ What is immunotherapy and how does it differ from chemotherapy?
Immunotherapy is a cancer treatment that stimulates the body’s own immune system to fight cancer, while chemotherapy uses chemical substances to kill rapidly dividing cells—both cancerous and healthy. Immunotherapy is generally more targeted and may have fewer side effects compared to chemotherapy.
❓ How does immunotherapy work?
Immunotherapy works by reactivating or strengthening the immune system’s natural ability to detect and destroy cancer cells. It helps overcome the defense mechanisms that cancer cells use to evade immune responses.
❓ Which cancers can be treated with immunotherapy?
Immunotherapy is effective in treating several cancer types, including:
- Non-small cell lung cancer
- Melanoma
- Kidney cancer
- Bladder cancer
- Hodgkin lymphoma
- Head and neck cancers
- Certain colorectal, gastric, and breast cancers (in selected cases)
Its use depends on specific biomarkers and the patient’s cancer profile.
❓ What are the main types of immunotherapy?
The five main types are:
- Immune checkpoint inhibitors
- T-cell transfer therapy (e.g., CAR-T cells)
- Monoclonal antibodies
- Cancer vaccines
- Immune system modulators (cytokines like IL-2 and IFN-α)
Each has a different mechanism and use case depending on the cancer type.
❓ Is immunotherapy suitable for all cancer patients?
No. Immunotherapy is not yet effective for all cancer types or patients. Suitability is typically determined by tumor biomarkers, PD-L1 levels, genetic mutations, and overall immune system function.
❓ How is immunotherapy administered?
Depending on the drug and cancer type, immunotherapy can be administered through:
- Intravenous (IV) infusion
- Oral medication
- Topical creams
- Intravesical (directly into the bladder)
Your oncologist will decide the most appropriate method and schedule.
❓ What are the most common side effects of immunotherapy?
Common side effects include:
- Fatigue
- Skin rash and itching
- Diarrhea
- Flu-like symptoms
- Inflammation of organs (e.g., lungs, thyroid)
More severe but less common side effects include cytokine release syndrome, neurological complications, and autoimmune reactions.
❓ How long does immunotherapy treatment last?
It varies depending on the type of cancer, stage, response to treatment, and the drug used. Some patients receive immunotherapy for a few months; others may continue for years under maintenance protocols.
❓ How is treatment response monitored?
Doctors use:
- Imaging tests (CT, MRI, PET-CT)
- Blood work
- Clinical evaluation of symptoms
Responses can be delayed with immunotherapy, so regular follow-ups are essential even if early changes are not seen.
❓ Can immunotherapy cure cancer?
While immunotherapy may not be a definitive cure for all cancers, it has led to long-term remission in many patients, especially in cases like melanoma or certain lymphomas. It is particularly promising in patients whose cancers did not respond to conventional treatments.
❓ Is immunotherapy safe?
Yes, immunotherapy is generally safe when managed by experienced oncologists. However, it must be carefully monitored due to the risk of immune-related side effects. Any unusual symptoms should be reported promptly.
❓ Can immunotherapy be combined with other treatments?
Yes. In many cases, immunotherapy is combined with chemotherapy, radiation, targeted therapy, or surgery to enhance treatment outcomes. Your oncologist will determine the best combination based on your case.